IADR Abstract Archives
Correlation of pressure and displacement during gingival retraction: an in vitro study
Objectives: There are numerous gingival displacement materials on the market; however, there is limited information available regarding the pressures that can atraumatically produce sufficient gingival displacement for a successful impression. This study uses an innovative model to measure pressure and the resulting movement of artificial gingiva.
Methods: Material and methods. An idealised tooth model was made from acrylic, and vinyl polysiloxane was used to simulate the free gingiva, sulcus, and attachment. The pressure and displacement achieved by three materials (Expasyl, Expasyl New, and KnitTrax Cord) was measured. A stereoscopic digital measuring microscope was used to quantify the space generated by the displacement material. A pressure gauge was used to measure the corresponding pressures, while Chart 5 software using a Power Lab system recorded the data.
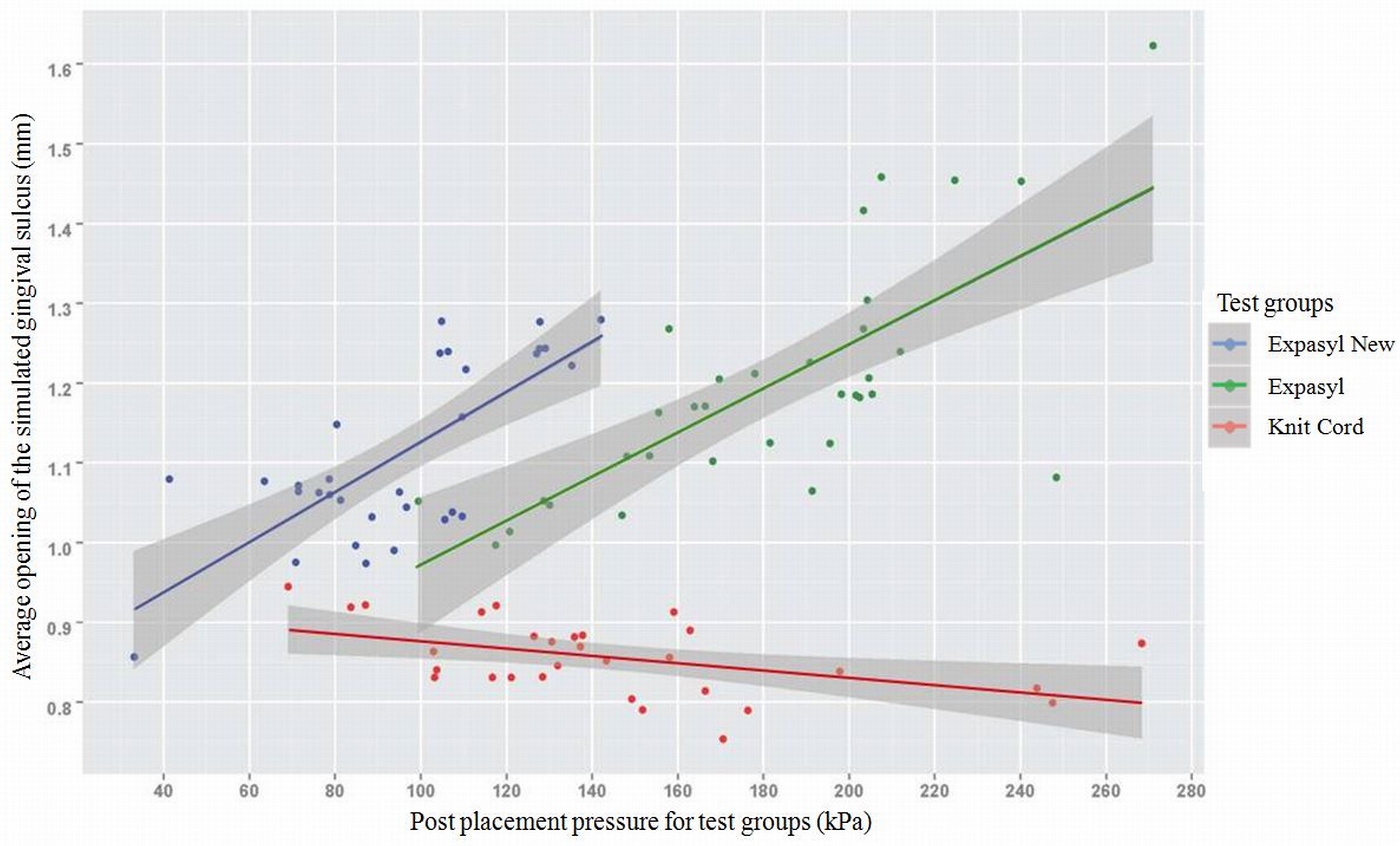
Results: Injection of Expasyl resulted in a retraction distance of 1.31 mm, Expasyl New produced 1.07 mm, and placement of KnitTrax Cord generated a 0.85 mm, which mirrors an ideal clinical outcome. The correlation between pressure and gap identified that Expasyl and Expasyl New behaved similarly while the KnitTrax Cord was different. Expasyl, Expasyl New and KnitTrax Cord all had maximum pressures that would be considered to be atraumatic to the epithelium attachment.
Conclusions: An increase in pressure resulted in an increase in displacement for the two paste materials; however, contrary to expectation, there was a decrease in displacement as pressure increased for the KnitTrax Cord. All retraction materials produced similar pressures below traumatic levels.
Methods: Material and methods. An idealised tooth model was made from acrylic, and vinyl polysiloxane was used to simulate the free gingiva, sulcus, and attachment. The pressure and displacement achieved by three materials (Expasyl, Expasyl New, and KnitTrax Cord) was measured. A stereoscopic digital measuring microscope was used to quantify the space generated by the displacement material. A pressure gauge was used to measure the corresponding pressures, while Chart 5 software using a Power Lab system recorded the data.
Results: Injection of Expasyl resulted in a retraction distance of 1.31 mm, Expasyl New produced 1.07 mm, and placement of KnitTrax Cord generated a 0.85 mm, which mirrors an ideal clinical outcome. The correlation between pressure and gap identified that Expasyl and Expasyl New behaved similarly while the KnitTrax Cord was different. Expasyl, Expasyl New and KnitTrax Cord all had maximum pressures that would be considered to be atraumatic to the epithelium attachment.
Conclusions: An increase in pressure resulted in an increase in displacement for the two paste materials; however, contrary to expectation, there was a decrease in displacement as pressure increased for the KnitTrax Cord. All retraction materials produced similar pressures below traumatic levels.