IADR Abstract Archives
A Fast Biodegradable Thiol-acrylate Hydrogels as a Cell Carrier for Stromal-cell Assisted Cranial Regeneration
Objectives: The objective of this study is to evaluate the in vivo bone formation induced by bone marrow- and dental pulp-derived stromal cells encapsulated in two thiol-acrylate hydrogels of different degradation rates in rabbit cranial defects.
Methods: Two formulations of biodegradable thiol-acrylate hydrogels based on 5 and 15 wt% polyethylene glycol diacrylate (PEGDA) were used. Bone marrow and dental pulp stromal Cells (BMSCs and DPSCs) were harvested from donor rabbits, isolated, expanded and then photoencapsulated in the hydrogel. The samples were then incubated in basal (BSL) or osteogenic (OST) medium. The cell viability and differentiation were analyzed using AlarmaBlue and ALP assay. In the animal study, fifteen New Zealand White Rabbits were used. The rabbits were divided into the following three groups: (1) BMSCs or DPSCs in 5wt% PEGDA hydrogels (n=5 rabbits), (2) BMSCs or DPSCs in 15wt% PEGDA hydrogels (n=5 rabbits) and (3) control group of returned bone plug, empty defects and 5wt% and 15 wt% PEGDA hydrogel without cells (n=5 rabbits). Six weeks post-implantation, the samples were retrieved, scanned with micro-CT, sectioned and stained for histological analysis.
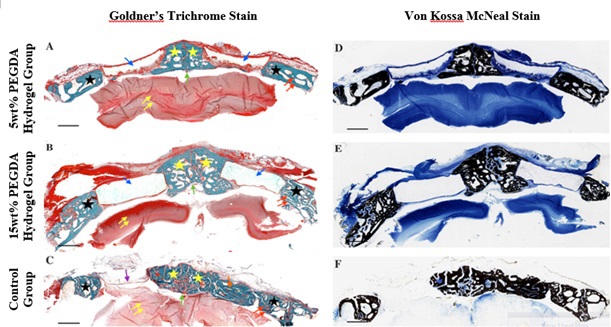
Results: AlamarBlue cell viability assay revealed significantly higher levels of cell viability in 5wt% PEGDA hydrogel compared to 15 wt% PEGDA hydrogel in both types of MSCs. Conversely, 15wt% PEGDA groups demonstrated significant increases in ALP activity at day 7 compared to 5wt% PEGDA hydrogel groups in both types of MSCs. In the animal study, micro-CT images show bone formation from the periphery and in the middle of the defects. Histological analyses revealed that the 5wt% PEGDA hydrogel resulted in lower averaged residual gel area and higher averaged bone formation compared to 15wt% PEGDA hydrogel specimens and the control groups.
Conclusions: Stem cells encapsulated in fast-degrading thiol-acrylate hydrogel can potentially be an effective way to repair large cranial defects.
Methods: Two formulations of biodegradable thiol-acrylate hydrogels based on 5 and 15 wt% polyethylene glycol diacrylate (PEGDA) were used. Bone marrow and dental pulp stromal Cells (BMSCs and DPSCs) were harvested from donor rabbits, isolated, expanded and then photoencapsulated in the hydrogel. The samples were then incubated in basal (BSL) or osteogenic (OST) medium. The cell viability and differentiation were analyzed using AlarmaBlue and ALP assay. In the animal study, fifteen New Zealand White Rabbits were used. The rabbits were divided into the following three groups: (1) BMSCs or DPSCs in 5wt% PEGDA hydrogels (n=5 rabbits), (2) BMSCs or DPSCs in 15wt% PEGDA hydrogels (n=5 rabbits) and (3) control group of returned bone plug, empty defects and 5wt% and 15 wt% PEGDA hydrogel without cells (n=5 rabbits). Six weeks post-implantation, the samples were retrieved, scanned with micro-CT, sectioned and stained for histological analysis.
Results: AlamarBlue cell viability assay revealed significantly higher levels of cell viability in 5wt% PEGDA hydrogel compared to 15 wt% PEGDA hydrogel in both types of MSCs. Conversely, 15wt% PEGDA groups demonstrated significant increases in ALP activity at day 7 compared to 5wt% PEGDA hydrogel groups in both types of MSCs. In the animal study, micro-CT images show bone formation from the periphery and in the middle of the defects. Histological analyses revealed that the 5wt% PEGDA hydrogel resulted in lower averaged residual gel area and higher averaged bone formation compared to 15wt% PEGDA hydrogel specimens and the control groups.
Conclusions: Stem cells encapsulated in fast-degrading thiol-acrylate hydrogel can potentially be an effective way to repair large cranial defects.