IADR Abstract Archives
Peri-implant Bone Dimensions Using Non-invasive Real-time Ultrasonography
Objectives: Peri-implant bone loss is the hallmark of failing dental implants affected with peri-implantitis. Intraoral 2-D radiographs are limited in only displaying interproximal peri-implant bone levels. Cone-beam computed tomography (CBCT) provides cross-sectional images but scattering artifacts reduce image quality. The aim of this human cadaver study was to examine the accuracy of high-resolution and 3-dimensional ultrasound to measure peri-implant bone dimensions.
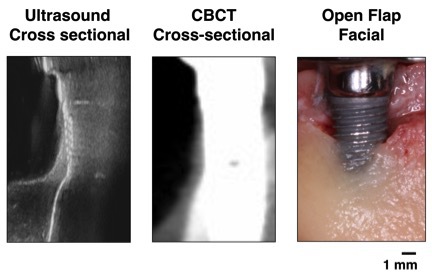
Methods: A prototype 25-MHz ultrasound probe was utilized via a precision positioner to scan peri-implant tissues of 17 implants from 7 fresh human cadavers. The marginal bone level and thickness were measured at mesio-, mid- and distal-facial sites. The ultrasound readings were compared to CBCT and direct, open bone measurements.
Results: The mean ultrasound, CBCT and direct marginal bone level readings were 2.58 ± 1.74, 2.82 ± 2.24, and 2.62 ± 1.78 mm, respectively. The corresponding mean marginal bone thickness was 0.93 ± 0.81, 1.19 ± 0.75 mm, and 0.96 ± 1.85 mm, respectively. The correlations (r) between the ultrasound and direct/CBCT readings of the 2 parameters ranged from 0.85 to 0.98 (p<0.0001). The mean absolute difference (95% CI) in marginal bone level between ultrasound and direct/CBCT was 0.035 mm (-0.61 to 0.68 mm, p=0.46) and 0.24 mm (-2.60 to 2.10 mm, p=0.16). The mean absolute difference (95% CI) in marginal bone thickness between ultrasound and direct/CBCT was 0.033 mm (-0.61 to 0.67 mm, p=0.56) and 0.23 mm (-0.99 to 0.56 mm, p<0.05).
Conclusions: This pre-clinical study showed encouraging evidence that ultrasound can measure peri-implant bone dimensions accurately with comparable values to open measures and CBCT. Validation of ultrasonography of peri-implant structures by clinical trials may offer potential of this non-invasive imaging technology to evaluate peri-implant tissue stability in 3-dimensions longitudinally without concerns of radiation exposure and imaging artifacts around implants.
Methods: A prototype 25-MHz ultrasound probe was utilized via a precision positioner to scan peri-implant tissues of 17 implants from 7 fresh human cadavers. The marginal bone level and thickness were measured at mesio-, mid- and distal-facial sites. The ultrasound readings were compared to CBCT and direct, open bone measurements.
Results: The mean ultrasound, CBCT and direct marginal bone level readings were 2.58 ± 1.74, 2.82 ± 2.24, and 2.62 ± 1.78 mm, respectively. The corresponding mean marginal bone thickness was 0.93 ± 0.81, 1.19 ± 0.75 mm, and 0.96 ± 1.85 mm, respectively. The correlations (r) between the ultrasound and direct/CBCT readings of the 2 parameters ranged from 0.85 to 0.98 (p<0.0001). The mean absolute difference (95% CI) in marginal bone level between ultrasound and direct/CBCT was 0.035 mm (-0.61 to 0.68 mm, p=0.46) and 0.24 mm (-2.60 to 2.10 mm, p=0.16). The mean absolute difference (95% CI) in marginal bone thickness between ultrasound and direct/CBCT was 0.033 mm (-0.61 to 0.67 mm, p=0.56) and 0.23 mm (-0.99 to 0.56 mm, p<0.05).
Conclusions: This pre-clinical study showed encouraging evidence that ultrasound can measure peri-implant bone dimensions accurately with comparable values to open measures and CBCT. Validation of ultrasonography of peri-implant structures by clinical trials may offer potential of this non-invasive imaging technology to evaluate peri-implant tissue stability in 3-dimensions longitudinally without concerns of radiation exposure and imaging artifacts around implants.